 |
| Daily health checks for the patient after the transplant |
Challenging, but it had to be succeeded
On March 2, upon receiving news from the National Organ Transplant Coordination Center about a brain-dead donor in Ho Chi Minh City, Prof. Dr. Pham Nhu Hiep, Director of Hue Central Hospital, activated the organ coordination system. Doctors were dispatched to collaborate with Gia Dinh People's Hospital and the National Organ Transplant Coordination Center to retrieve the organs.
However, due to weather conditions, the airline delayed the flight, making everyone anxious. Dr. Nguyen Duc Dung, (MSc.) Head of the Department of Cardiothoracic Surgery at the Cardiovascular Center of Hue Central Hospital, recalled: “The flight was originally scheduled to depart early in the day, but because of the fog, it didn’t could not take off until noon, making the team retrieving the heart extremely anxious. Thanks to the smooth coordination between the units, as soon as we arrived, we immediately began dissecting the heart. At 4:10 p.m. that day, the heart was on its way. The police escorted the vehicle, clearing all traffic jams, so within just 7 minutes, the donated heart arrived at the airport in time to catch the afternoon flight back to Hue.”
This was an unforgettable transplant case for the doctors and medical team. The recipient was Mr. N.V.C, 36 years old, residing in Quang Nam. He had been in an accident six years ago and was diagnosed with dilated cardiomyopathy and end-stage heart failure, with an ejection fraction (EF) of 20% and pulmonary artery pressure (PAPs) ranging from 75-80 mmHg. Mr. C. is 1.75 meters tall and weighs 89 kilograms, which was fairly similar to the donor's physique. According to doctors at Hue Central Hospital, he was the heaviest recipient with the highest pulmonary pressure among all heart transplant cases across Vietnam, posing a major challenge for the transplant team - especially in terms of anesthesia and post-operative resuscitation. “A high PAPs index leads to the risk of heart failure due to increased pulmonary artery pressure, so the doctors had to carefully plan and prepare treatment strategies post-transplant. Running ECMO (extracorporeal membrane oxygenation) was necessary to support the patient at that time,” shared a member of the transplant team.
Although faced with many difficulties, if the transplant was not carried out, the patient would never have had another chance, as it is extremely rare to find a heart suitable for someone with such a large physique. The mission to save the patient's life placed a heavy responsibility on the doctors, compelling them to make every effort to ensure the transplant's success.
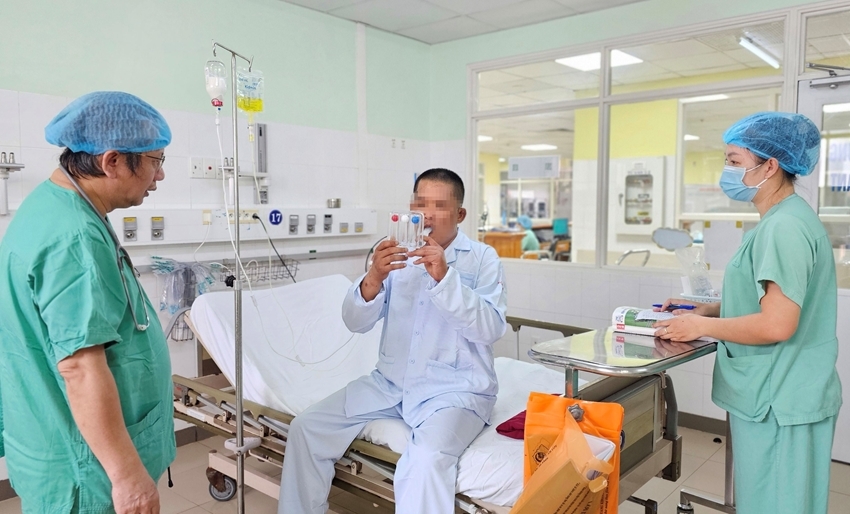 |
| The patient practiced breathing exercises in the special monitoring room |
After 3 hours and 48 minutes from the moment it was removed from the donor's chest, the heart began beating its first rhythms inside the body of the man from Quang Nam. Following the surgery, the patient was transferred to the intensive care unit for continued critical care: he was sedated, placed on mechanical ventilation, administered medications to treat heart failure and pulmonary hypertension, and maintained on ECMO. Due to severe heart failure and high pulmonary artery pressure after the transplant, the intensive care team used medications to strengthen cardiac contractions and dilate the pulmonary arteries, along with the ECMO system, successfully weaning him off extracorporeal circulation.
Dr. Dang The Uyen, Specialist Level II, Deputy Director of the Cardiovascular Center and Head of the Department of Anesthesiology and Intensive Care, shared: “This case was almost like an emergency heart transplant situation on a patient with end-stage heart failure due to dilated cardiomyopathy. The patient had experienced life-threatening arrhythmias multiple times and had to have an implantable cardioverter-defibrillator (ICD) placed. The high pulmonary artery pressure posed many challenges during the transplant procedure. Fortunately, thanks to the seamless coordination, modern equipment that met the demands of difficult resuscitation scenarios, and intensive treatment, the transplanted heart is now functioning well. The patient’s hemodynamics are completely stable, and he can eat on his own and perform light movements in the ICU bed.”
One life comes to an end, but many others are renewed
Earlier, on the evening of March 1st, Mr. C.G.C (an ethnic Nung from Ho Chi Minh City) was in a serious accident. Despite receiving emergency treatment at Gia Dinh People’s Hospital, his condition did not improve. After being counseled, his family agreed to donate his heart, liver, and kidneys, saving five patients suffering from organ failure across the three North, Central, and South regions of Vietnam. Mr. C.P.L., his father, shared: “This is a tremendous loss for us, but we tried to hold back our pain and agreed to donate his organs. Although our son is gone, we hope that many other patients will have the chance to continue living - that is also a comfort to our family.”
Receiving the heart of a stranger, the first moment he regained consciousness, Mr. N.V.C. felt his chest lighter than before. Once a tour bus driver and the main breadwinner of his family, heart failure had turned him into a burden. His wife left, and his young child had to be raised by his elderly parents. “The joy is indescribable. I feel much healthier now, and after every meal, I even drink milk,” he shared. “Though I don’t know who donated their heart, I sincerely want to thank his family for giving me a second chance at life. When I return home, I will find a job to support my child’s education and help my parents repay our debts,” he confided.
 |
| Mr. N.V.C. couldn’t hold back his tears when he reunited with his mother after 10 days in the hospital room |
In the intensive care unit after his heart transplant, Mr. N.V.C. practiced breathing exercises and took gentle steps under the guidance of doctors and nurses. Upon seeing his mother again after the surgery, he burst into tears like a child, even though he is already the father of a 7-year-old son. His elderly mother comforted and reassured him, saying: “Just being alive is a blessing, my child!”
Mrs. Vo Thi Khiem, the mother of the heart transplant patient, recalled the moment she was picking vegetables when she received a call from the doctors telling her to prepare for the transplant. She and her son hurriedly took a bus to Hue to complete the necessary paperwork. When the staff at Hue Central Hospital’s Organ Transplant Center consulted and explained the situation to her, she cried non-stop, unable to remember anything clearly - only instinctively responding, “I’m so worried! Please use the best medicine, I beg you all to save him!” The mother from Quang Nam shared, “After his accident, his wife left him. I had to raise both my son and my grandchild, who was only 25 months old at the time. To afford treatment for my only son, my husband and I agreed to borrow from everywhere we could and sell whatever we had left to save him. Now, there are no words to express my gratitude!”
One life came to an end, but instead of being consumed by grief, their family bravely chose to "give" - bringing new life to five others. That body did not return completely to dust, but continued to sow the seeds of life, spreading humanity and kindness throughout the community.